
- CATARACT
- GLAUCOMA
- REFRACTIVE ERRORS
- SQUINT
- DIABETIC RETINOPATHY - A silent presence
- AGE RELATED MACULAR DEGENERATION (ARMD)
- UVEITIS
- TERMS IN GENERAL EXAMINATION

- CATARACT
- GLAUCOMA
- REFRACTIVE ERRORS
- SQUINT
- DIABETIC RETINOPATHY - A SILENT PRESENCE
- AGE RELATED MACULAR DEGENERATION (ARMD)
- UVEITIS
CATARACT
What is Cataract?
Normally, the lens of the eye is clear and allows light rays to pass through easily. When a cataract develops, the lens becomes cloudy and opaque. The light rays no longer pass through the lens easily, so the patient cannot see clearly.
- Cataract is not a new growth or a film over the eye. In most cases, it is just part of the aging process.
- It is not contagious

Types Of Cataract
There are many types of cataracts.
A change in the chemical composition of the lens
causes most cataracts. The following are the various types of cataracts.
- Senile cataract
This is the most common type of cataract, comprising 80 percent of the total cataracts. It occurs in patients above the age of 50.
- Congenital Cataract
Cataracts in children are rare. They can be caused by infection of the mother during pregnancy, or they may be hereditary.
- Traumatic Cataract
Eye injuries may cause cataracts in patients of any age.
- Secondary Cataract
Eye diseases, like glaucoma, iritis, eye tumours, and diabetes may cause cataracts.
- Drug-induced Cataract
Prolonged treatment with steroid drugs, either for local (e.g., allergic conjunctivitis) or systemic diseases (e.g., asthma) may lead to cataract formation.
Symptoms of Cataract
- Blurring or dimness of vision
- Feeling of a film over the eyes
- Sensitivity to light and glare
- Change in colour of pupil
- Double vision and dulling of colour sense

Treatment
Cataract cannot be cured by medicines or spectacles. Removal of the clouded lens through surgery is the only treatment.
Types of Cataract Removal
- Routine method (old method)
After administering a local anesthesia, a 10 mm incision is made in the eye. The cataract lens is removed and it may be replaced by an Aphakic glass. The incision is then closed with sutures. After the surgery, glasses with high power called aphakic spectacles are prescribed to the operated person.
- Disadvantages:
These aphakic glasses are heavy, images seen are larger than they normally appear to be, and the field of vision is restricted.
- New method (IOL) - Implanting of Intraocular lens (IOL) with sutures:
After administering a local anaesthesia, a 10 mm incision is made in the eye. The clouded lens is removed and replaced by an IOL and the incision is then closed with sutures. The entire procedure takes only 15 minutes.
What is IOL?
Intra Ocular lens (IOL) is a tiny transparent convex lens. It is made of polymethyl methacrylate , (a harmless plastic substance). Unlike contact lens, an IOL stays permanently in the eye and does not cause irritation.
Advantages of IOL
- Since the lens is placed inside the eye, most often the patient need not wear glasses
for clear vision. But sometimes patient has to wear glasses for clarity. - Images are clear and of the same dimension without distortion
- Full vision returns very clearly
- Normal field of vision
Phaco or suture less surgery with implantation of IOL
After giving a local anaesthesia, a 5mm incision is made in the eye. The cataract lens is broken into small pieces by a machine with ultrasonic waves and removed with a needle.
A specially prepared IOL is inserted into the eye and the wound heals without sutures.
Advantages of Phaco
- Early surgery can be done, so that patient need not wait for the cataract to mature
- Small Incision
- No sutures and no need of suture removal.
- No irritation, no watering
- Early return to work
- No need to continue drops for a long time
- No need for hospital stay, Even if the patient stays, it is only for a short time
- Only one post-operative visit
- Stable refraction after one month
The ophthalmic surgeon decides whether the patient can undergo Phaco or not

GLAUCOMA
Glaucoma is a condition wherein the pressure of fluid within the eye (hydrostatic pressures within the eye) gradually increases to a level not tolerated by the sensitive tissues of the eye. The optic nerve, which is similar to a cable wire carrying visual images to the brain, is the portion of the eye susceptible to damage from glaucoma. Such damage is irreparable and visual loss due to glaucoma is irreversible.

Causes of Glaucoma
There is a fluid filled chamber in the front of the eye called the anterior chamber. It is filled with aqueous humour, which bathes and nourishes the tissues of the eye. If the drainage of this fluid is restricted, for reasons yet unknown, pressure builds up within the eye causing glaucoma.
Who is likely to get Glaucoma ?
- Persons over the age of 40 are more likely to develop glaucoma. However, the disease may occur in people of all ages including newborns.
- Persons with myopia, diabetes, systemic hypertension and family history of glaucoma have an increased risk.
Symptoms of Glaucoma
In most cases of glaucoma, the patient is not aware of the gradual loss of sight until vision is significantly impaired.
However, if glaucoma progresses without adequate treatment, the following symptoms may occur in some individuals:
- Pain around the eyes when coming out from darkness (e.g., as soon as the person comes out of a cinema hall)
- Coloured halo rings seen around light bulbs especially in the mornings and nights
- Frequent change of reading glasses, headaches, pain and redness of the eyes
- Reduced vision in dim illumination and during nights
- Gradual decrease of side vision with progression of glaucoma
- Blurring of vision
How is Glaucoma treated ?
A simple test with a device called the tonometer measures pressure within the eye. This test alone cannot detect all glaucomas. The back of the eye should be inspected to view the optic nerve after dilating the pupils. Side vision may also be examined by a computer-assisted, simple test called perimetry (visual field examination).
The loss of vision due to glaucoma is irreversible. However, appropriate treatment and regular follow-up can preserve residual vision.
Earlier the diagnosis, better the chances of arresting visual impairment.
Medications
For most people with glaucoma, regular use of medications will control the increased fluid pressure. However, in some, drugs may stop working after a period of time. In these situations, the ophthalmologist can help by adding or changing medications or by choosing another type of treatment: laser or surgical methods. Periodical eye examinations are therefore essential to ensure that the medications are working.
- Laser treatment
In some type of glaucomas, called angle closure glaucomas, laser treatment is the primary form of reducing the eye pressure. This is a simple out-patient procedure, which uses a strong beam of light to relieve the fluid pressure. In open angle type glaucomas, laser treatment is applied only if various medications fail to control the fluid pressure. Medications need to be continued regularly even after laser treatment. Laser treatment has very minimal complications, but its effect in reducing the eye pressure may wear off over time.
- Surgery
In some persons with glaucoma, medical or laser treatment is insufficient to arrest glaucoma and surgery is indicated. But this treatment option has its risks and limitations and is reserved as the treatment of last resort. Even after surgical treatment, individuals with glaucoma should continue periodical check-ups by an ophthalmologist and additional medications may be required indefinitely.
REFRACTIVE ERRORS
In normal vision, light rays from an object focus on the retina (emmetropia). Alternatively, in the presence of a refractive error, the light rays get focused in front or behind the retina causing blurred vision. Under normal conditions, as the eye ball grows in size from infancy to adulthood, there will be a corresponding change in curvature of cornea and the lens enabling the eye to remain emmetropic, at all ages.
When one of these fails to happen, refractive error occurs:
- The eye ball being larger or smaller than the normal size
- The corneal curvature being flatter or steeper than usual
- Increase or decrease in the power of the lens

These refractive errors can be classified as myopia (near sightedness) and hyperopia (far sightedness)
What is hyperopia ?
In hyperopia or far sightedness, the light rays from an object form an image behind the retina.
Children with hyperopia
- Find difficulty in reading, writing and looking at both near and distant objects.
- Eye strain while trying to read for long hours
- May have squint (crossed eyes)
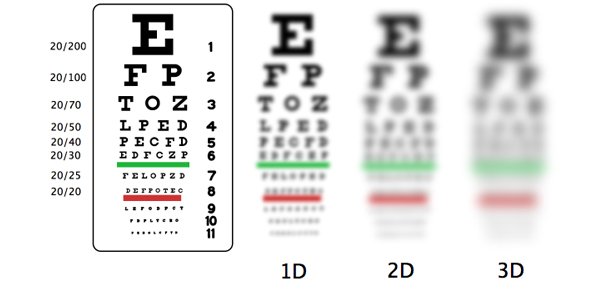
What is myopia ?
In myopia or near sightedness, the light rays from an object form an image in front of the retina.
Children with myopia
- Have defective vision for distance and clear vision for near
- Squeeze their eyes while trying to see distant objects
- Hold books close to their face while reading
- Pain, watering or burning sensation in the eyes, rub their eyes constantly or blink frequently, because of the eye strain which they experience all the time
- Headache in the forehead region intensified in the evening
- Recurrent swellings in the eye lids.
Children with the above conditions may also have
Treatment for the above conditions
- Corrective spectacle is the best option available. Though children may initially refuse to accept glasses, they will become fond of them once they realise they can see better with them on.
- The power of the glasses may change depending on the growth of the eye ball. An eye check-up and change of glasses if necessary, has to be done once in 6 months for children under 5 years of age and once a year thereafter. Making a child wear glasses regularly is the duty and responsibility of the parents.
- Failure to wear glasses in childhood when needed will retard the development of vision in that eye.
- Children older than 15 years can use contact lenses if they don't want spectacles. Those over 18 to 20 years of age with stable power also have the option of Lasik, a laser refractive surgery apart from contact lenses.
Failure to correct the refractive errors and the eventual low vision may hamper the academic activities of the child. So an ophthalmic consultation is essential in children, especially with symptoms of refractive errors. Finally, there is no relationship between nutritional deficiency and the occurrence of refractive error. So loading these children with Vitamin A will not help them. Sometime this may lead on to other complications.
SQUINT
Squint is misalignment of the eyes such that the right and left eyes are pointed in different directions. Though it is a common condition among younger populations, affecting 2 to 4 percent of children, it may also appear later in life.
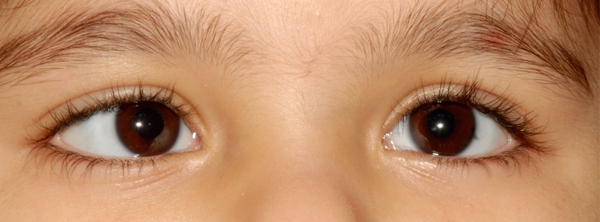
The misalignment may be permanent or it may be temporary, occurring occasionally. The deviation may be in any direction: inward, outward, upward or downward.
Causes
- Weakened muscles or abnormal nerve impulses to the eye muscles
- Heredity
- Blurred or poor vision
- Pathology inside the eye, such as cataract
Signs and Symptoms
The primary sign of squint is an eye that is not straight. Sometimes, a youngster will squint or close one eye in bright sunlight. Faulty depth perception may be present. Some children turn their faces or tilt their heads in a specific direction in order to use their eyes together.
- Treatment
Parents often get the false impression that a child may "outgrow" the problem. If a child's two eyes are pointed in different directions, examination by an ophthalmologist is necessary to determine the cause and to begin treatment.
The goals of treatment are to preserve vision, straighten the eyes and to restore binocular vision. Treatment of squint depends upon the exact cause of the misaligned eyes. It can be directed towards unbalanced muscles or other conditions which are causing the eyes to point in two different directions. After a complete eye examination, including a detailed study of the inner parts of the eye, an ophthalmologist can recommend appropriate optical, medical or surgical therapy.
- Non surgical treatment - spectacles
Some squints are caused by refractive errors. In such cases, squint can be corrected by prescribing proper spectacles.
- Surgical treatment

Pre operative

Post operative
Most patients require surgical correction. Surgery is done under general anesthesia in children and under local anesthesia in cooperating adults. To undergo general anesthesia the child should be free from acute illness. Parents should inform the doctor if the child is having any systemic problems such as cardiac disease or epilepsy.
- Routine investigations before surgery include a blood test and an X-ray of the chest.
- Surgery is done either on both eyes simultaneously or on one at a time.
- Surgery is done on eye muscles situated outside the eyeball The principle of surgery is to weaken the stronger muscle and strengthen the weaker muscle. Either one or several muscles may be operated upon, depending on the type and severity of squint.
- Eye is bandaged for one day after surgery.
- After surgery, eye drops are to be used for one month.
- Oral medication is not required except in a few cases.
- Hospital stay is only two days.
- First follow-up is one month after surgery.
- If amblyopia is present frequent follow-up appointments for a longer duration are required.
- It is unnecessary to restrain the normal activity of the child.
Diabetic Retinopathy
An increasing incidence of diabetes mellitus poses a major health problem in India. The contributing factors are:
- an inappropriate diet, high in fat and carbohydrates
- sedentary lifestyle
Diabetes may affect both the young (type I) and the old (type II). The latter type is far more common. Regardless of the type of diabetes, many diabetics develop a complication called diabetic retinopathy, a change in the retinal blood vessels that leads to loss of vision.
Diabetic Retinopathy - A silent presence
- Diabetics are twice as likely as non-diabetics to develop eye problems . The most common eye complication in diabetes is diabetic retinopathy; other complications are cataract and glaucoma.
- Fifty percent of diabetics develop some degree of diabetic eye disease.
- The risk of blindness is 25 times higher in diabetics than in non-diabetics.
- Early detection and timely treatment of diabetic eye disease significantly reduces the risk of vision loss.
- Diabetic retinopathy is often symptom less in the early stages. Since only an ophthalmologist can detect early signs of diabetic retinopathy, all diabetics should have their eyes examined at least once every year.
How does diabetes affect the eye ?
Diabetes causes weakening of the blood vessels in the body. The tiny, delicate retinal blood vessels are particularly susceptible. This deterioration of retinal blood vessels, accompanied by structural changes in the retina, is termed diabetic retinopathy and will lead to loss of vision.
Diabetic retinopathy is gradual in onset and is related to the duration of diabetes. High blood glucose levels, high blood pressure and genetics influence the development and progression of diabetic retinopathy.
There are two main stages of diabetic retinopathy:
- Non-proliferative: When the blood vessels leak, macular edema may occur, thereby reducing vision.
- Proliferative: When new, weak blood vessels grow or proliferate, bleeding into the vitreous may occur and cause severe visual loss.
Eye examination in diabetic retinopathy
Every diabetic is a potential candidate for diabetic retinopathy. There are no symptoms at the initial stages. Periodic eye examination with dilated pupils is the only way to detect early disease and prevent further deterioration of vision.
Diagnostic
Diagnostic tools such as a slit lamp, ultrasound and procedures such as fluorescein angiography are used in addition to an ophthalmoscope to assess whether the patient has diabetic retinopathy or other eye problems.
Fluorescein Angiography
This is a magnified photography of the retina using an injectable dye. It helps classify the condition, record changes in the retinal blood vessels, decide on the mode of treatment and evaluate the treatment.
Treatment
Lasers are widely used in treating diabetic retinopathy. Lasers are formed by an intense and highly energetic beam of light. They can slow down or stop the progression of diabetic retinopathy and stabilise vision.
- The laser experience
Laser treatment is usually performed as an outpatient procedure. The patient is given topical anaesthesia to prevent any discomfort and is then positioned before a slit lamp. The ophthalmologist directs the laser beam precisely on the target with the aid of the slit lamp and a special contact lens. Absorption by the diseased tissue either seals or destroys the tissue. Additional treatment may be required according to the patient's condition.
Side effects
Some patients may experience side effects after laser treatment. These are usually temporary. Possible side effects include watering eyes, mild headache, double vision, glare or blurred vision. In the event of sudden pain or vision loss, the ophthalmologist must be contacted immediately.
Vitrectomy
In some patients, there may be bleeding into the vitreous or the vitreous may pull the retina, reducing vision severely. In such instances a surgical procedure called vitrectomy (replacing the vitreous by a clear artificial solution) is performed. Vitrectomy is done only after other forms of treatment have been unsuccessful.
Age Related Macular Degeneration (ARMD)
Macular degeneration is a condition of the eye that is often related to aging. It is commonly referred to as age-related macular degeneration, and is often abbreviated as AMD. Age related macular degeneration is the most common cause of legal blindness in the geriatric population in the west and is probably more common in India than believed.
What is amblyopia ?
Amblyopia is reduced vision in an anatomically normal eye. The term "lazy eye" is used to describe it.
When does amblypia develop ?
Amblyopia develops when any of the following conditions occur:
- Squint/Strabismus (eyes not positioned straight)
- There is a difference in power between the two eyes (one eye focuses differently from the other)
- Cataract (clouding of the lens)
- High or moderate power in both eyes
- Severe ptosis (droopy eyelids)
- Children under 9 years of age whose vision is still developing are at the highest
risk for amblyopia. Generally, the younger the child is, greater is the risk.
Why does amblyopia develop ?
Amblyopia develops because when one eye is turned, as in squint, two different pictures are sent to the brain. In a young child, the brain learns to ignore the image of the deviated eye and see only the image of the better eye. Similarly when there is difference in power between the two eyes, the blurred image formed by the eye with greater power is avoided by the brain. In order that the retina may capture an object, it needs adequate light and visual stimulus. When these factors are absent, as in the presence of cataract, amblyopia results. A moderate or high degree of refractive power present in both eyes, when not corrected early and adequately, also results in amblyopia.
- What should be done ?
Amblyopia can often be reversed if it is detected and treated early. Cooperation of the patient and parents is required to achieve good results. If left untreated or if not treated properly, the reduced vision or amblyopia becomes permanent and vision cannot be improved by any means.
- How is amblyopia treated ?
The most effective way of treating amblyopia is to make the child use the amblyopic eye. Covering or patching the good eye to force the use of the amblyopic eye may be necessary to ensure equal and normal vision. This can be achieved by:
- Prescribing proper spectacles if the patient is found to have refractive error
- Removal of cataract when indicated
- Occluding the normal eye
- Surgery, when amblyopia is accompanied by strabismus
- Occlusion refers to closure of the normal eye with a patch, thus forcing the child to use the amblyopic eye. Occlusion is done from a few hours to a few days, depending upon the age of patient and the type and severity of amblyopia. In cases experiencing less severe amblyopia, partial occlusion, such as that by making one glass translucent, may be sufficient. Older children can do reading exercises at home while patching the normal eye. Those patients who are patching their eyes need periodic follow-up, which is scheduled with an ophthalmologist. Duration of treatment may extend from months to years. The ophthalmologist will decide for how long the occlusion should be continued. Loss of vision from amblyopia is preventable if treatment is begun early.
Facts on patching
- Patching is not a pleasant thing for a child, so initially the child will be reluctant to undergo it. It is our duty to make the child understand the necessity of the procedure so that he/she will cooperate.
- In a young child patching is done for shorter periods initially; the duration is increased gradually to obtain better compliance.
- Acceptance is good as soon as vision is increased in ambloypic eye.
- Method of patching should be according to the interests of the child
- Patch should be stuck directly on the face over the eye.
- If the child wears glasses, the patch should be placed on the face, not on the glasses.
- Glasses can also be used as an occluder only in older children.
- Many children try to take the patch off. This problem usually disappears as the child grows accustomed to wearing the patch.
- Older children can be encouraged to read and young children can be involved in playing interesting games during patching.
- Precautions must be taken to prevent the child from peaking around the edge of the patch.
- Patching schedules should be followed strictly.
- Patching should not be stopped abruptly. The programme should be tapered only by ophthalmologists.
- Regular follow-up visits are a must.
Uveitis
The eye is shaped like a ball with three different layers. The outer layer is the sclera, the innermost is the retina, and the middle layer is the uvea. Uveitis is the inflammation of the uvea.
Impact of Uvetis
The uvea nourishes the eye through blood vessels. Diseases of the uvea thus affect the nutrition of vital structures: the cornea, lens, retina, and vitreous. Uveitis may threaten sight and is more serious than other common eye disorders.
Symptoms of Uveitis
- Light sensitivity
- Blurred vision
- Pain
- Redness of the eye
Causes of Uveitis
- Systemic inflammatory diseases such as multiple joint pains
- Systemic diseases like tuberculosis, syphilis, and leprosy
- Trauma or injury to the eye
- Virus, fungal or bacterial illness of the eye
- Idiopathic uveitis - unknown causes
Types of Uveitis
There are different types of uveitis depending on which part of the eye is affected:
- When the uvea is inflamed near the front part of the eye it is called anterior uveitis, which usually has a sudden onset and may last 6-8 weeks.
- If the uvea is inflamed in the middle of the eye, it is called intermediate uveitis and affects the muscle that focuses the lens.
- Inflammation in the back of the eye is called posterior uveitis; it has a slower onset and may last longer than other types of uveitis.
- When the inflammation affects the anterior, intermediate and posterior zones it is called panuveitis.
Acute presentation
Certain types of uveitis start suddenly. Patients may suffer from severe pain, redness and defective vision. Uveitis can disappear with proper treatment.
Chronic presentation
When uveitis is present for one year, certain cases can be cured with treatment, while others can only be controlled.
Diagonis of Uveitis
A careful examination of the body and eye by an ophthalmologist is extremely important when symptoms occur. Inflammation can affect sight and lead to blindness if not treated. Since uveitis may be associated with diseases in other parts of the body, the ophthalmologist should take a complete health history. He or she may need to consult the patient's primary care physician or other medical specialists.
Treatment of Uveitis
Uveitis is a serious eye condition that may cause permanent scars. Immediate and appropriate treatment is the secret to success. Treatment with steroids and pupil-dilating eye drops, with or without systemic medications, is necessary.
Uveitis - special problems
- Uveitis is underestimated as a cause of blindness in most blindness surveys.
- Accurate treatment of uveitis is possible only when an etiological diagnosis is made.
- The conventional treatment of uveitis of unknown origin with systemic corticosteroids can be harmful in areas where HIV, tuberculosis and leprosy are endemic.
- Uveitis is associated not only with visual disability but also with systemic diseases, and therefore is with increased morbidity.
Recent developments in the diagnosis of uveitis has shown that an etiological diagnosis can be established in 70 percent of uveitis patients. Increasing awareness of uveitis, conducting proper workups and treating the disease may bring down the incidence of blindness due to uveitis.
Terms you may come across when general examination is being done
Vision testing: Vision testing involves making a person read standard sized letters at a specified distance. The doctors record the vision as a fraction e.g. 6/6 etc. The top number denotes the distance (in feet) at which the patient has been able to read the particular sized letter while the bottom number indicates the distance at which a normal person is expected to read the same letter. Near vision is tested separately in good illumination using special test charts held at normal reading distance. The testing is done with each eye separately. The doctors often test the vision using a pinhole. This gives an estimate of improvement possible with glasses. The patient in place of glasses cannot use the pin

Auto Kerato Refrecto Meter

Slit lamp with Applanation Tonometer
Refraction: This is an important test that is done by the ophthalmologist or more often by the optometrist. The eye is like a camera. The light rays are focused on to the light sensitive film in the back of the eye called the retina. This focusing is made possible by the cornea (a clear watch glass like structure in the front of the eye) and by the lens in the eye (similar to the lens of a camera). Refraction is done usually in the normal state. On occasion (especially in children) it may have to be done using special eye drops (cycloplegics). In this situation one may have to retest the power of the required glasses 2-3 days after the testing with the use of drops. Refraction involves two parts. The first part is objective where in the refractionist estimates the power needed by using a test called retinoscopy. This test can also be done with a machine called the automatic refractometer (so called computer testing). However one still needs to do the all-important subjective testing (i.e. testing the response of the patient with different powered glasses) before.
Dilatation: One of the most common procedures that is done in an eye specialist's office is dilatation. The pupils of the eye constrict or dilate depending upon the light that thrown at the eye. For examining the back part of the eye (fundus), the doctor uses an instrument called ophthalmoscope. To get a good view of the back of the eye, one needs to dilate the pupils. This permits more light to enter the eye and gives a better image of the fundus. To keep the pupils dilated despite the intense light, one needs to dilate the pupils. There are various types of dilating drops available. The faster acting ones may dilate the pupil in 15-20 minutes time. Other variety of drops may take up to 30-45 minutes for good dilatation. The effect of dilatation usually lasts up to 6 hours. Some of them may retain the effect for 24 hours. Usually the drops used for routine eye examination do not have long lasting effect. A patient is expected to have glare in the sun light while still under the effect of the drops. Hence driving may become difficult. If you had similar dilatation in the past and have been noted to be allergic to any one of them, please inform the same to your doctor.

